 Serologic Tests: The anti-AChR Ab test is very specific, and it confirms the diagnosis in patients with classical clinical findings. The laboratory investigations and procedures usually aid the clinician in confirming the clinical findings. 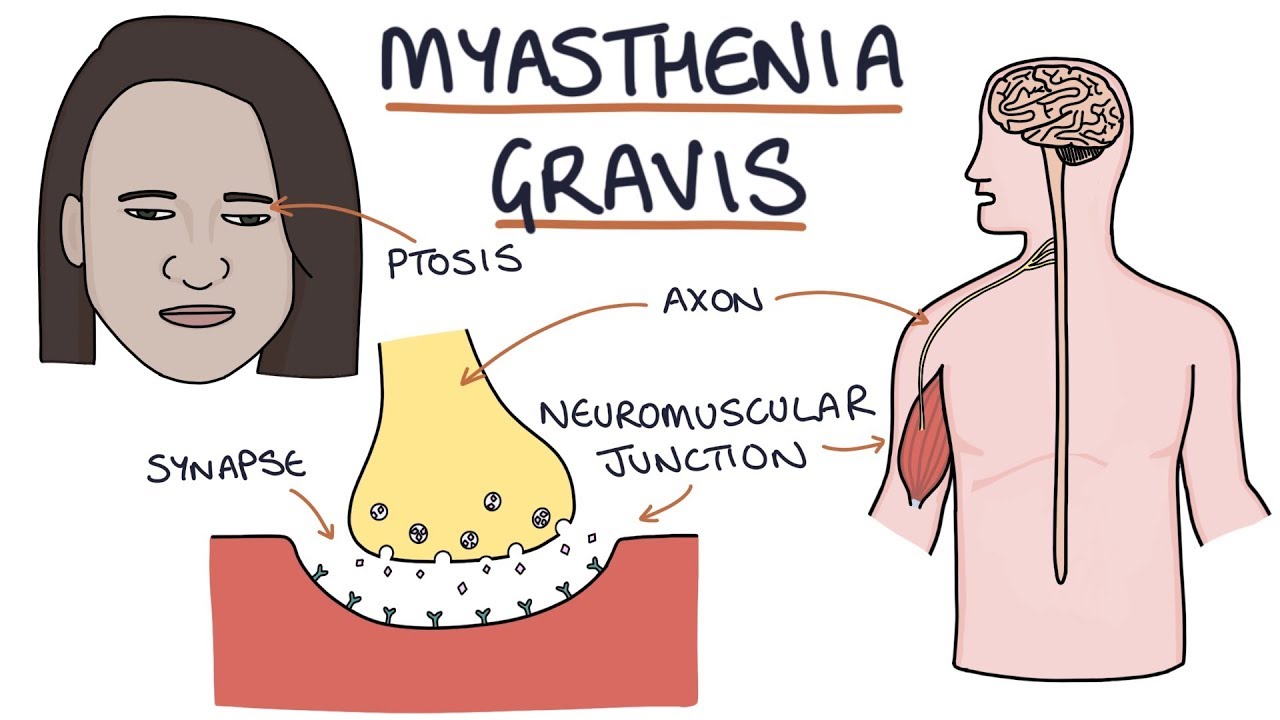
Each class carries different prognoses or responses to therapy. Ĭlinical Classification: The Myasthenia Gravis Foundation of America (MGFA) clinical classification divides MG into 5 main classes based on the clinical features and the disease severity. Myasthenic crisis is also frequent in the MuSK MG. It is more common in females, relatively spares extraocular muscles, and commonly involves bulbar, facial, and neck muscles. MuSK MG has clinical features that are quite different from n-AChR MG. The pupils, deep tendon reflexes, and sensory examinations are normal. Improvement is seen after a period of rest or application of ice (ice-pack test) to the muscle group involved. In such cases, repeated or sustained muscle contractions can demonstrate weakness. The physical examination may reveal normal muscle power because of the fluctuating disease pattern. There are no autonomic symptoms like palpitations, bowel, or bladder disturbances that occur in MG as it only involves the nicotinic cholinergic receptors. Myasthenic crisis: It is due to the involvement of intercostal muscles and diaphragm and is a medical emergency. The ACh released at the nerve terminal, in turn, is unable to generate the postsynaptic potential required to generate an action potential in muscle due to a reduced number of n-ACh receptors leading to the symptoms of muscle weakness. The weakness is more pronounced with the repeated use of a muscle group since it causes depletion of the ACh store in the NMJ. The inhibition of the complex leads to a reduced number of n-ACh receptors. They bind to the Agrin–LRP4–MuSK protein complex in the NMJ, whose primary function is the maintenance of the NMJ, including the n-ACh receptor distribution and clustering. In MusK MG and LPR4 MG, the antibodies are of the IgG4 subtype and do not have the complement activating property. They may also act by functionally blocking the binding of ACh to its receptor or by enhancing the endocytosis of the antibody-bound n-ACh receptor. MAC brings about the final degradation of the receptors. They bind to the n-ACh receptor present in the postsynaptic membrane of the skeletal muscles and activate the complement system leading to the formation of the membrane attack complex (MAC). 
In n-AChR MG, the antibodies are of the IgG1 and IgG3 subtype. The pathophysiologic mechanisms in MG are dependent on the type of antibodies present. These include myasthenic crisis, an acute respiratory paralysis that requires intensive care, as well as adverse events due to long term medication treatment like opportunistic infections and lymphoproliferative malignancies.Ī complete understanding of the pathophysiologic mechanisms, clinical manifestations, treatment strategies, and complications of myasthenia gravis is necessary for better patient care and outcomes. Myasthenia gravis causes a significant number of complications. A wide variety of conditions can precipitate MG, such as infections, immunization, surgeries, and drugs. The reduced transmission of electrical impulses across the neuromuscular junction due to the formation of autoantibodies against the specific postsynaptic membrane proteins consequently causes muscle weakness. It usually involves muscles of the eyes, throat, and extremities. The classic presentation is a fluctuating weakness that is more prominent in the afternoon. Myasthenia gravis (MG) is the most common disorder affecting the neuromuscular junction (NMJ) of the skeletal muscles. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
